Cost-Effectiveness in Healthcare: Enhance Quality to Optimize Spending
Cost-effectiveness in healthcare doesn’t have to compromise service quality. By increasing effectiveness, you can enhance the services provided while reducing costs.
As technology advances and offers new opportunities within the healthcare ecosystem, even small adjustments to daily processes can save time and money, all while improving patient safety.
In this article, we will cover several angles on how technology might make your hospital (and especially the OR) more cost-effective without compromising quality. You will find topics such as:
We believe that this short guide will help you be more cost-effective by improving the quality of the healthcare services you are delivering.
What is cost-effectiveness in healthcare?
Cost-effectiveness in healthcare is the process of examining both cost and health outcomes. However, healthcare costs are a delicate topic. You are trying to manage how much is spent, but you don’t want to compromise good patient care. Over everything else you want patients to have the best quality of life.
It is a common thought that by managing costs you are reducing the quality of the goods and services you deliver or use. While this might be true in some cases, often a big slide in healthcare spending has to do with the items you need and protocols you’ve to apply.
A practical case for this matter was the COVID-19 pandemic, where spending grew drastically because of the personal protective equipment (PPE) needed. This was especially in the first months when information was scarce and surgeons would operate in full disposable suits.
However, regardless of the healthcare spending, controlling the pandemic was a matter of public health. You were not reducing the quality of the healthcare services you provided – it was the other way around. But the equipment required increased and these were in some cases not reimbursed by health insurance.
COVID aside, the same thing happens in the day-to-day activities of your hospital. You are using, storing, and buying more items than those you need – especially in the surgical ward.
The good news is that technology can help you manage costs.

How can technology assessment control health spending?
As we have already introduced, using technology might lead to reducing your healthcare spending. Even if you don’t have any idea of how databases, big data, AI, and other technologies work in the background you may still use them to your advantage.
To make it easier for you we will be exploring 3 cost sources and how can technology assessment control health spending:
Reduce Surgical Instrument tray costs
Surgical instrument tray costs are one of the first strategies that can increase the efficiency of an operating room and technology can have a huge impact on it.
Have you ever wondered how much it costs to sterilize an instrumentation tray and how many you need per surgery?
-
Sterilizing 1 instrument tray may cost around $75.
-
A TKA may need 8 instrument trays. This means $600 per procedure and, for an average of 700k surgeries, $420M a year.
-
THA may need around 14 instrument trays. This means $1050 per surgery and an average of $420M per year if you do around 400k surgeries.
The point is that the surgeon ends up only using half of the material that is prepared and this is where you use technology to reduce your healthcare costs.
When preparing for surgery, if you don’t know what to expect, you are likely to overprepare on instrumentation ready to use. However, each tray that is not used still has to be sterilized.
Using Artificial Intelligence, PeekMed allows orthopedic surgeons to predict what implant (and size) they will need for each procedure before the case starts and enters the OR.
As each implant requires different instruments to implement, if you know exactly what you will need, you will only prepare the instruments you should be using.
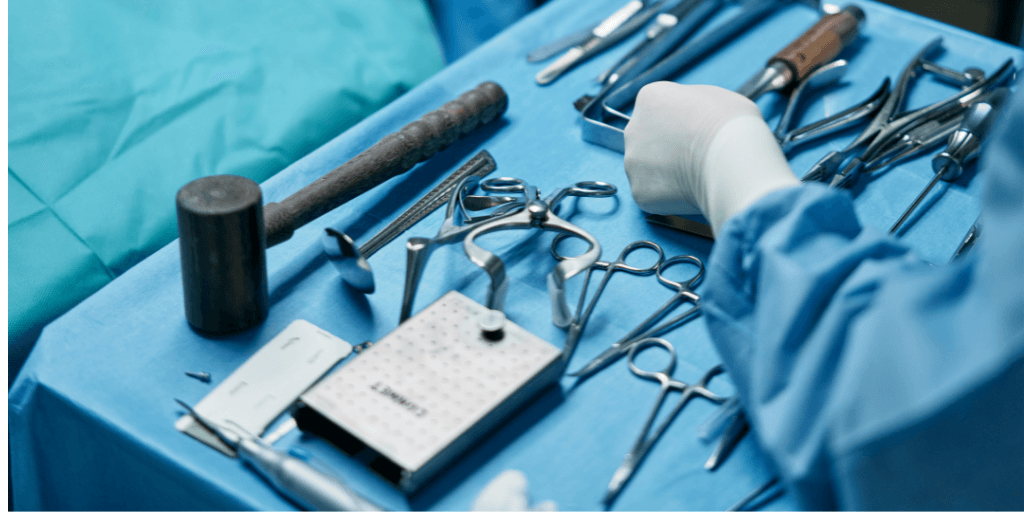
Achieve cost-effectiveness in healthcare by reducing storage needs
The same process happens if you manage the implants you will need – as you reduce the required storage. If you know what size and brand you are using, you can order and store fewer items.
Even if these are consigned to you by the implant manufacturer, remember that storage has huge costs – especially in the era of the supply chain crises, due to COVID and the war in Ukraine.
In practical terms, what happens is that PeekMed allows you to take full advantage of the health system technology you already have in your hospital.
Reading data from the imaging devices, you will be provided with insights that would be only available once the surgery has already started.
This is only one of the advantages of orthopedic digital templating.
Improving turnover: time is money
The use of technology also leads to reduced surgery and turnover time.
The points we’ve suggested earlier in this article might appear that you are adding an extra step to your already busy schedule. But studies show that by doing this you are reducing surgery time by 20% to 50%.
Knowing the implant brand and size, surgeons do not have to try out several options and since all the suggestions take into account data from other surgeries, may even suggest an implant you don’t normally use.
This leads to an improvement in surgical floor usage and reduces the turnover time. While a good old analog preoperative planning might seem a perfect solution, studies show that doing it digitally might save you up to 39% time planning, too.
Improving the quality of healthcare with technology
If you know what instruments and implants you’ll be needing, you are not only improving your logistics and managing healthcare spending. You are providing a patient-centered approach too.
Accessing this data and information is a good strategy to prevent complications such as shoulder osteoarthritis or incomplete recovery (incomplete restoration of joint motion), studies suggest.
Hence, the existence of preoperative planning can have relevant benefits for the patient, as it may prevent surgical errors.
Being cost-effective does not mean that you have to stop delivering high-quality healthcare. It can increase it.

